
Hi, I’m Alyssa! AKA, The PCOS Nutritionist Alyssa!
I’m a Registered Dietitian dedicated to helping you eliminate your PCOS symptoms with sustainable and realistic nutrition changes.
Some of Our Favorite Products
PCOS and Ovulation Tests: The Best Way To Use Them
- This post may contain affiliate links.
Tracking ovulation can be tricky when you have PCOS, especially if your cycles are irregular. As a registered dietitian who struggled with infertility due to PCOS, I understand the struggle.
In this blog post, we’ll break down everything you need to know about PCOS and ovulation tests, including why they can be confusing, how to use them more effectively, and any other alternatives that may be useful. Whether you’re trying to conceive or just want to understand your cycle better, you’re not alone in navigating this.

What Is Ovulation?
Ovulation is a phase in your menstrual cycle when a mature egg is released from the ovary. The egg then travels down the fallopian tube where it can potentially be fertilized by sperm. Ovulation typically happens about midway through your cycle. So for someone with a 28 day cycle, ovulation may occur around day 14.
There are two outcomes that can occur after ovulation. First, the egg can be fertilized by sperm and eventually implanted into the lining of the uterus. This will result in a positive pregnancy test. The second potential outcome is the egg is not fertilized and your hormone levels drop as your body prepares to shed the uterine lining. This will lead to your period starting.
Ovulation is a key part of fertility, but it’s also a sign of overall hormonal health. Regular ovulation is important for every menstruating woman.

How Does PCOS Impact Ovulation?
Polycystic ovary syndrome (aka PCOS) can significantly impact ovulation by disrupting the hormonal signals that regulate your menstrual cycle. In a typical cycle, rising levels of hormones like FSH and LH trigger the growth and release of a mature egg. But with PCOS, there’s often a hormonal imbalance that can interfere with this process, especially higher levels of androgens (aka male hormones like testosterone levels) and insulin levels.
As a result, ovulation may happen less frequently or not at all. This is why many women with PCOS have irregular periods or absent periods altogether. It’s also why many people with PCOS struggle with fertility or have a hard time tracking their cycles. In fact, PCOS is one of the most common causes of infertility.
In short, PCOS doesn’t mean you never ovulate. It means that ovulation may be unpredictable or delayed for some people, and that makes tracking and timing a bit more challenging.
PCOS and Ovulation Tests: Are They Reliable?
PCOS and ovulation tests can be tricky. The hormonal imbalances associated with PCOS may interfere with the accuracy of these tests. Ovulation tests work by detecting the luteinizing hormone (LH) surge. The LH surge typically occurs about 24 to 36 hours before ovulation. Usually, when someone sees a positive result with their ovulation tests, it gives them a heads up that ovulation is about to happen in the next 1 to 2 days.
Since women with PCOS often don’t ovulate regularly (or at all), they usually have high levels of LH throughout their cycle. The high LH levels can result in false positives or inaccurate readings on ovulation test strips. Some women with PCOS may see multiple positive LH tests within one cycle. This is usually because the body is trying to ovulate and seeing the normal hormone fluctuations, but then it just isn’t quite able to actually ovulate.
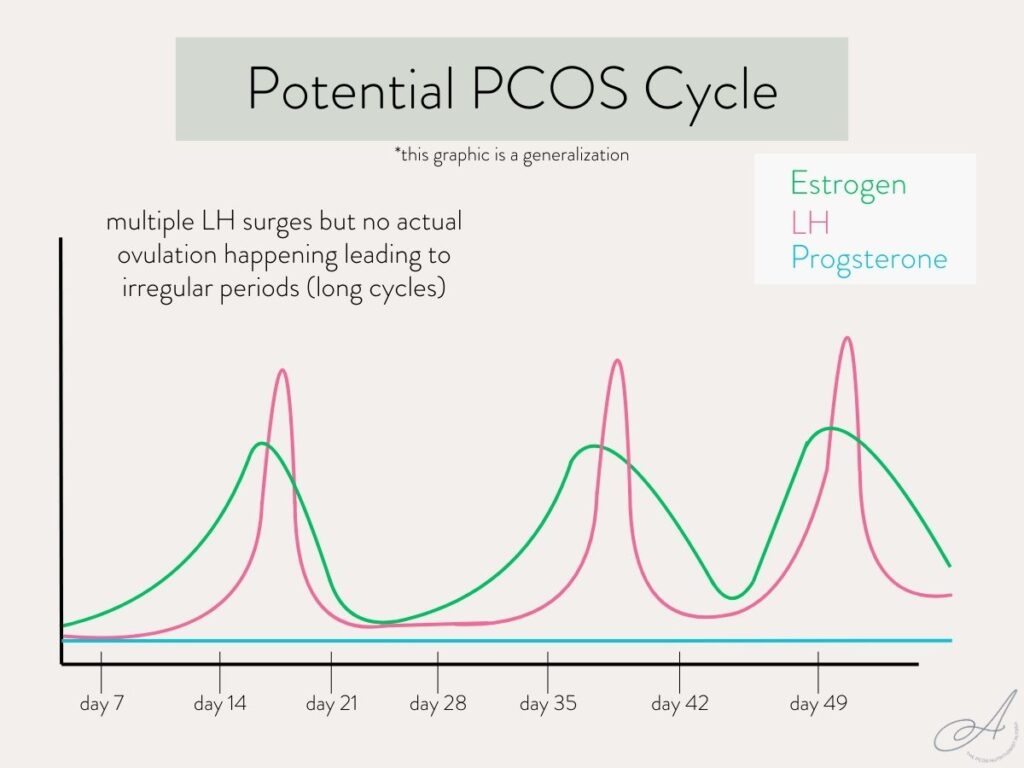
Additionally, because ovulation may not occur regularly in those with PCOS, it can be challenging to pinpoint the right window for testing – leading to almost daily testing. Obviously, this can create a lot of frustration with ovulation tests.
Ultimately, ovulation tests can still be helpful in tracking patterns, but they may not be as reliable for predicting ovulation in PCOS.
Tracking Ovulation with PCOS
While ovulation tests may not be a reliable method to use for predicting ovulation, they may still be a useful tool for some people. For more accurate results though, combining ovulation tests with other tracking methods can improve the chances of identifying ovulation accurately.
At Home Ovulation Tracking Methods for PCOS
There are several at-home methods for ovulation tracking. Which method you choose will depend on your current needs and goals.
Basal Body Temperature (aka BBT)
After ovulation occurs, your progesterone levels increase. Progesterone is thermogenic, meaning it increases your core body temperature (aka your basal body temperature or BBT). It’s a very slight increase, usually an increase of only 0.5 to 1.0 degrees Fahrenheit.
In order to monitor ovulation with BBT, you’ll need a specific BBT thermometer. You can find very affordable ones online. This is best for people with regular sleep schedules since you do need to take your temperature every morning at the same time before you actually get out of bed. If this doesn’t sound feasible, I’d highly recommend a wearable device like Tempdrop. I have used Tempdrop for years and love it. You can read my full Tempdrop review here.
Something that’s extremely important to note is that BBT tracking will only confirm that ovulation did actually occur. It does not predict that ovulation may be occurring in the next 1 to 2 days. If you’re trying to conceive and you’re not in tune with other ovulation symptoms, you may miss your fertile window if you’re only tracking your BBT.

Cervical Mucus Changes
Another sign of ovulation is changes in cervical mucus (you may have commonly heard this referred to as discharge). As ovulation gets closer, you may notice that your cervical mucus gets slippery and sticky. The color may change to clear or slightly cloudy – usually resembling raw egg whites. This type of cervical mucus is usually referred to as egg white cervical mucus.
Because of hormonal fluctuations with PCOS, a chance in cervical mucus can sometimes still be a false positive. It’s best to pair this with other ovulation tracking methods to help you predict and/or confirm ovulation occurred.
Ovulation Predictor Kits
We talked about these ovulation test kits already. They can often cause false positive results with PCOS because of chronically high LH levels or multiple LH surges without ovulation. If you’re trying to conceive and decide to use these ovulation strips, it’s usually smart to also pair other ovulation tracking methods.
Urine PdG Tests
At-home urine PdG tests measure a urine metabolite of progesterone. After ovulation, progesterone levels rise and your body will also have PdG in your urine. Unlike LH tests that can give false positives without ovulation occurring, PdG will only be present if ovulation occurred.
The downside of these is that if you have PCOS and irregular cycles, it may be frustrating to figure out whether you should be using LH tests or PdG urine tests.
Fertility/Hormone Monitors
In the past several years, several fertility monitors have popped onto the market. As someone who has personally tried a few of these devices, they are pretty impressive and take the guesswork out of tracking your cycles.
If you’re considering investing in something like this, Inito is my top pick for an at-home fertility monitor.
Inito measures 4 different fertility hormones:
- FSH: tracks follicle growth
- Estrogen: usually rises 3-4 days before ovulation and 1-3 days before LH levels rise
- LH: surges 24-36 hours before ovulation
- PdG: rises after ovulation (note: PdG is a urine metabolite of progesterone, not progesterone itself)
Inito uses a urine sample and takes just 10 minutes to help you identify your 6 day fertile window and also confirm that you’ve ovulated. While the other options discussed so far can only potentially predict ovulation is going to occur or that ovulation has occurred, Inito combines these two key pieces of information.
Unlike traditional OPKs though, Inito actually catches the true LH surge which leads to ovulation. This is particularly helpful for those of us with PCOS since it’s pretty common to have elevated LH levels or multiple LH surges in a single cycle.
Inito also has extra perks like a free phone app that does the heavy lifting for you. It interprets your hormone trends and gives you clear prompts when you’re experiencing high fertility and peak fertility days. So if you’re trying to conceive, this can significantly increase your chances of getting pregnant.
The downside to these types of devices is the cost, but if it’s within your budget, these can take the guesswork out of your fertility journey.
If you’re interested in trying Inito, use this link or enter code ALYSSA15 at checkout. It’s even HSA/FSA eligible!
Medical Ovulation Tracking Methods for PCOS
Of course, there are medically supervised methods to tracking ovulation if you have PCOS. These are typically used when someone is trying to conceive and has been unsuccessful.
The two most common methods are:
- Blood tests – your healthcare provider or fertility specialist may opt to test certain hormones such as estradiol, LH, FSH, or progesterone to predict or confirm ovulation.
- Ultrasound – your health care provider may perform ultrasounds to predict or confirm ovulation. Ultrasounds can visualize follicles and immature eggs and even the release of an egg depending on the timing in your cycle.
Now that you know some options for predicting your fertility times and confirming ovulation with PCOS, let’s talk about how you can regulate your periods and achieve more regular ovulation.
Improving Ovulation Rates with PCOS
I know that it can be really frustrating and disheartening if you have irregular menstrual cycles or you’re not ovulating regularly (or at all) with PCOS…especially if you’re trying to get pregnant. There are some healthy changes you can make that can greatly improve ovulation rates and your chances of conceiving.

Optimize your Diet
Insulin resistance, chronic inflammation, and higher levels of androgens (such as testosterone) are known contributors to symptoms of PCOS, including irregular cycles.
Here’s a few dietary strategies that you can focus on:
- Stable blood sugar levels. Combine sources of protein, complex carbohydrates, and healthy fats at each meal. This combo keeps blood sugar levels more stable and can improve menstrual regularity and egg quality.
- Omega 3 fatty acids. Increase your intake of foods rich in omega 3 fatty acids such as chia seeds, flax seeds, hemp seeds, walnuts, and fatty fish like salmon, herring, or trout.
- Zinc rich foods. Foods rich in zinc can also improve ovulation and lower testosterone levels. Oysters, cashews, pumpkin seeds, yogurt, oats, and beef are all good sources of zinc.
- Vitamin D rich foods. Vitamin D is a hormone that plays a vital role in the menstrual cycle. Fortified dairy, salmon, eggs, and sunlight are good sources of vitamin D.
For tips on how to put this all together, grab your copy of a 7 Day PCOS Diet Plan PDF here.
Make Lifestyle Changes
Certain lifestyle changes can also improve your hormone balance and increase your chances of conceiving. Adequate physical activity, or regular exercise, is always a good idea. This can be as easy as walking or yoga. Additionally, getting enough sleep and managing stress levels are incredibly beneficial too.

Medications or Supplements
Your doctor may prescribe certain medications to help you such as Metformin, Clomid, or Letrozole.
Additionally, there are some dietary supplements that have been well researched for PCOS. Inositol is the most well studied PCOS supplement and can help to improve menstrual cycles in many scenarios. Some women with PCOS may be inositol-resistant and benefit from the addition of alpha-lactalbumin to help enhance inositol absorption and achieve regular periods.
Read more about the benefits of inositol here: Ovasitol Benefits for PCOS. If you think you may be one of those people who are inositol-resistant or want to learn more about it, read this: Ovasitol vs Ovasitol Plus Alpha-Lactalbumin: Which is Best?
The Bottom Line
PCOS and ovulation tests are not as straightforward as one might think. Ovulation strips measure the LH surge, which occurs about 24 to 36 hours before ovulation occurs. With PCOS, LH levels may be chronically elevated, which can create a lot of false positives, confusion, and heartbreak.
If you choose to use ovulation tests and have PCOS, I’d recommend combining them with another type of ovulation tracking method such as basal body temperature tracking, cervical mucus monitoring, PdG urine tests, or hormone monitors such as Inito or Mira. Additionally, your healthcare provider may choose to medically monitor your cycles with blood tests and ultrasound tracking.
Aside from monitoring your cycles and ovulation, your diet and lifestyle can make a big difference in how often you ovulate. Medications and supplements may also improve ovulation rates too.
Other Posts You’ll Love
Best Prenatal Vitamins for PCOS
Inositol vs Berberine for PCOS: Which Is Better?
PCOS Diet Plan to Get Pregnant
Disclaimer: this is for informational purposes only. It does not substitute for or replace professional medical advice for polycystic ovarian syndrome (PCOS) or any other medical condition. Always consult with your personal medical professional for personalized health advice.


